COMMUNITY ONSET CENTRAL LINE ASSOCIATED BLOODSTREAM INFECTIONS (CO-CLABSIS) IN PEDIATRIC ONCOLOGY PATIENTS: AN UNDERESTIMATED PROBLEM?
I. Kopsidas, S. Papachristidou, E. Kourkouni, M. Baka, A. Pourtsidis, G. Tsopela, M. Tsolia, S. Coffinusa, T. Zaoutis, D. Doganis, N. Spyridis.
36th Annual Meeting of the European Society for Paediatric Infectious Diseases (ESPID 2018)
Malmö, Sweeden, May 28- June 2, 2018
BACKGROUND: CLABSIs are a common complication in the inpatient pediatric oncology setting. CLABSIs are associated with significant mortality, morbidity, and healthcare costs. The majority of the literature focuses on CLABSIs in the hospital setting but less known about the epidemiology of CLABSIs in the pediatric oncology ambulatory setting(Community Onset CLABSIs:COCLABSIs). Our aim was to describe the burden and nature of COCLABSIs in children with cancer.
METHODS: A prospective study was conducted at large pediatric oncology hospital in Athens, Greece. All patients(12/2015-12/2017) with a central line(CL) and a bloodstream infection(BSI) within the first 48 hours of admission without a focus of infection, were prospectively studied. Patients discharged within 5 days prior to entry to the study were excluded. Clinical and demographic data including length of antibiotic therapy, central line removal, ICU admission within 72hours, chemotherapy delay and death within 30 days, were collected. CLABSI surveillance data were also collected for inpatients using CDC definitions.
RESULTS: Thirty-one COCLABSIs cases were identified with a median hospitalization duration of 10days(IQR: 6-11) and a median antibiotic course of 10 days(IQR: 10-10). The infection resulted in a delay in chemotherapy in 8/29(27.6%),catheter removal in 4/31(12.9%) and 1 patient 1/31(3.2%) required ICU admission. No deaths were recorded. During the same period,12 CLABSIs occurred in the hospital. Pathogens isolated are shown in Table1. Gram negative organisms were responsible for the majority COCLABSIs in contrast to CLABSIs which were caused predominately by Gram positive.
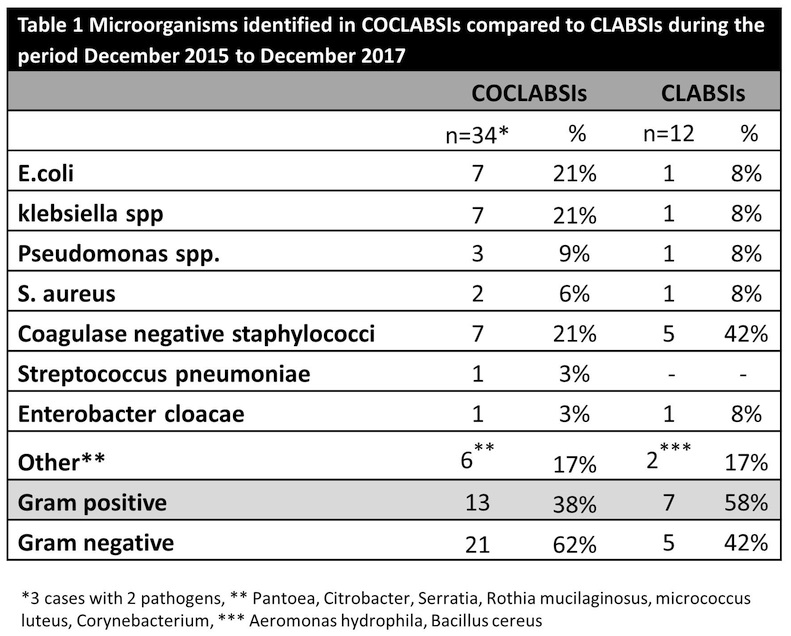
CONCLUSIONS: COCLABSIs were not uncommon in pediatric oncology patients in the ambulatory setting and were associated with significant morbidity including delays in chemotherapy for the underlying malignancy. The different pathogen distribution compared to hospital-acquired CLABSIs may provide clues to the pathogenesis and inform future prevention efforts for these infections.



