VENTILATOR-ASSOCIATED EVENTS IN THREE PICUS IN GREECE
E. Chorianopoulou, C. Barbaresou, E. Chorafa, E. Iosifidis, I. Kopsidas, E. Kourkouni, M. Machaira, I. Papadatos, C. Tsirogianni, G. Tsopela, T. Zaoutis E
37th Annual Meeting of the European Society for Paediatric Infectious Diseases (ESPID 2019)
Ljubljana, Slovenia, 6-11 May, 2019
BACKGROUND: Healthcare-associated infections (HAI) are associated with increased morbidity and mortality and excess costs. Ventilator-associated events (VAEs) are HAIs associated with prolonged mechanical ventilation and hospital death. The broad objective of this study was to develop a VAE collaborative in pediatric intensive care units and to present the results.
METHODS: We conducted active surveillance for VAE in three pediatric intensive care units (PICUs) in Greece from June 2016 to June 2018, using the Centers for Disease Control and Prevention’s National Healthcare Safety Network definitions from 2016. VAE definitions include ventilator-associated conditions (VAC) and subcategories for infection-related ventilator-associated complications (IVAC) and possible ventilator-associated pneumonia (PVAP). Data were collected and managed using REDCap electronic data capture tools.
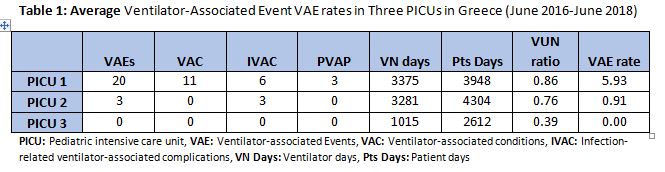
RESULTS: A total of 7671 ventilator days (VN days) and 10864 patient days (PT days) were analyzed. Twenty-three VAE were identified, of which 11 were VAC, 9 were IVAC, and 3 were PVAP. Ventilation utilization (VUN) ratios ranged from 0.39 to 0.86, and VAE rates ranged from 0.00 to 5.93. The events occurred at a median of 15 days (IQR:9-36) after intubation and patients remained on the ventilator a median of 18.5 days (IQR:7-42) after the event. Six of the 19 patients that experienced a VAE died; 4 died within 10 days of the event.
CONCLUSIONS: We established a surveillance mechanism that allows for a uniform description of VAE rates and ventilator utilization ratios in PICUs in Greece. This mechanism demonstrated considerable variability among these rates and ratios. These results will be used to inform the implementation of a care bundle.